Translate this page into:
What role can a homoeopathic psychiatrist play in restoring mental health in an unequal world?
-
Received: ,
Accepted: ,
How to cite this article: Dhawale KM. What role can a homoeopathic psychiatrist play in restoring mental health in an unequal world? J Intgr Stand Homoeopathy 2021;4:98-105.
Abstract
World Mental Health Day, observed on the 10 October, is an occasion for the mental health professionals to dedicate themselves to bringing succour to the numerous persons suffering from mental health disorders. The World Mental Health Federation has declared this year’s theme as ‘Mental Health in an Unequal world.’ The call is timely considering the distress wrought on different communities due to the pandemic and the social and economic distress which has affected all sections of the population, albeit with different intensities causing differing impacts. The article explores the theme in the historical context and outlines the various concerns which mental health professionals should concern themselves with. It is a common knowledge that they are in short supply all over the world. Homoeopaths, due to their approach to health, disease and individuals are uniquely equipped to fill this gap and thus make a difference. There are very few examples, at the institutional level, where community-based activities addressing the mental health issues have been successfully undertaken and have made an impact. The article draws on the almost two-decade-long experience of the Department of Homoeopathic Psychiatry, Dr. M. L. Dhawale Memorial Homoeopathic Institute in this area, thereby illustrating the possibility of incorporating similar practices in the District Mental Health Programme. Clinical activity needs to be reported in peer-reviewed journals and initiating research in priority areas would help homoeopathy to be recognised as a discipline which can be a part of Integrated Mental Health Care for mental disorders.
Keywords
District Mental Health Programme
School mental health
Community mental health workers
Senior citizens mental health
‘…there is no health without mental health’
WHO. Mental health: facing the challenges, building solutions. Report from the WHO European Ministerial Conference. Copenhagen, Denmark: WHO Regional Office for Europe, 2005
WORLD MENTAL HEALTH DAY
The World Federation for Mental Health (WFMH) is the only international multidisciplinary, grassroots advocacy and education organisation concerned with all aspects of mental health. The WFMH was founded in 1948, along with the United Nations (UN) and the World Health Organization (WHO). Its objectives are preventing mental and emotional disorders, advocating the proper treatment and care of those with such disorders and promoting mental health. Since 1992, the WFMH has celebrated 10 October as World Mental Health Day to draw attention of the world community to the importance of Mental Health. Since 1994, the day has been organised around a theme; this year, the theme is ‘Mental Health in an Unequal World.’
We aim to understand the significance of the theme in the light of the following observations:
The world is getting increasingly polarised – politically, racially, religiously, socially and economically. An easy and free dialogue between people of different groups is becoming increasingly difficult. The wealth gap is continually increasing as the rich become richer and the number of people living in poverty is still far too high. Inequality is rising in all countries
The events of 2020 have highlighted longstanding inequalities due to race and ethnicity, sexual orientation and gender identity and the lack of respect for human rights in many countries, including for people living with mental health conditions. Such inequalities have an impact on people’s mental health
The pandemic has exacerbated these differences immensely; no further example is needed once the global vaccine inequity is noted; Africa has hardly commenced administering the first dose, while Israel has started providing booster doses, having covered more than 60% of its population with the mandatory two doses.
The theme draws our attention to this inequity with respect to mental health services in our own country as well; we have seen traumatic events during the second wave, when health facilities were under stress for all people, rich or poor. We were also the unfortunate witnesses to inequity amongst the healthcare professions, where adherents of evidence-based sciences ruled the roost although the ‘evidence’ they produced to base their actions was flimsy. Homoeopaths were at the receiving end, having failed to convince the ‘powers that be’ of our credentials despite catering successfully to several epidemics through our 250-year history. The situation is similar while tackling the mental health pandemic. This article illustrates the significance of the problem of mental illness in our country and what we as homoeopaths, and particularly the small growing breed of homoeopathic psychiatrists, can achieve with sound training and efforts.
IMPORTANCE OF MENTAL HEALTH
The importance of Mental Health in our daily life and living needs no elaboration since the WHO has defined it ‘a state of well-being in which the individual realises his or her own abilities, can cope with the normal stresses of life, can work productively and fruitfully and is able to make a contribution to his or her community.’ Numerous advances in the importance of quality of life and the various factors which support it are our daily concerns. However, that mental health disorders can affect numerous medical conditions is not as well known.[1] Mental illness can influence a number of non-communicable diseases for example, depression can be a risk factor for stroke, diabetes or coronary disease and is often a consequence of these illnesses. Mental illness can significantly interfere with treatment compliance for several communicable illnesses as well for example, HIV/AIDS, tuberculosis and malaria. Most are aware of the close relationship between mental illness and suicide. However, the negative impact of maternal depression on child growth and development and its role in increasing infant mortality are relatively unexplored.
Prince et al.[2] stated that if effective treatment is provided to mothers with mental illness, the proportion of stunting in their children would progressively reduce; the degree of reduction is based on the proportion of mothers treated.
Thus, there is no doubt that there is no health without mental health. This is truly a Hahnemannian concept that we should strive to make an operational reality.
STATE OF MENTAL HEALTH IN INDIA TODAY AND ITS IMPACT
During 2014–2016, the National Institute of Mental Health and Neurosciences, Bengaluru, carried out an epidemiological survey on the current state of Mental Health in our country.[2] This National Mental Health Survey (NMHS) covered 12 states and approximately 34,000 individuals above the age of 18 years. The findings have been carefully aggregated and are revealing with regard to the prevalence, the sociodemographic characteristics, the nature of disorders and the availability of mental health resources to take care of the affected population. Some of the findings are as follows:
The prevalence of mental disorder is 10.6%, meaning one in 11 people needs help. However, a later study that covered population of all ages has put the figure higher at 14.3%[3]
Tobacco and alcohol abuse disorders are highly prevalent at 13.1% and 4.6%, respectively. Most individuals with these conditions do not consider their state as constituting a disorder at all and thus are unlikely to seek help
Common mental disorders are quite prevalent, including stress disorder (3.5%), affective disorder (2.8%) and depressive episode (2.7%). Thus, nine of 11 people have conditions that are quite treatable, if they can find suitable medical help. The prevalence of serious conditions such as schizophrenia and bipolar disorders is approximately 0.8%
Child mental health is a serious cause for concern as the estimated prevalence of idiopathic developmental intellectual deficit is a whopping 4.5%; conduct disorder, attention deficit hyperactivity disorders and autism spectrum disorders total 1.6%.[4] In a previous study, we found that the prevalence of learning disabilities in Marathi medium schools was 8.33%.[5] Based on these figures, we can determine the considerable difficulty our schools and teachers face when managing a class in which almost 10–12% need special attention.
Santomauro et al. estimated a significant increase in the prevalence of both major depressive disorders (MDDs) (with an estimated additional 53.2 million cases worldwide i.e., a 27.6% increase) and anxiety disorders (76.2 million additional cases i.e., a 25.6% increase) since before the pandemic.[6]
The economic burden is difficult to fathom. The proportion of disability proportion is relatively higher among individuals with bipolar affective disorders (63–59%), MDD (67–70.0%) and psychotic disorders (53–59%). Moreover, this is not confined to those affected but the family members too have to forego between 10 and 20 days to care for the affected family members.[3]
From the present, we move to the future. The estimation of trends over the next 10 years is not very promising. We are aware that the prevalence of non-communicable illnesses is rising globally. In low-income countries, the proportion of DALYs is set to increase from 35% in 2005 to 45.1% in 2030, while the contribution of neuropsychiatric disorders was set to marginally decrease from 26.1% to 24.4%.[1]
As is evident from the above, our society is mainly dealing with common mental disorders and substance abuse. When homoeopaths focus on the understanding and treatment of these conditions, we would be able to help a substantial number of those affected, and hence, homoeopathic institutions would do well to focus on these areas for training and research.
INEQUITY OF MENTAL HEALTH ACROSS POPULATIONS
Urban metros are becoming a pool for aggregation of mental conditions, more than rural or non-metro cities. The prevalence of neurotic or stress-related disorders (6.93%), mood disorders (5.6%) and schizophrenia and other psychoses (0.64%) was 2–3-fold greater in urban metros.[2] The prevalence of MDD, apart from its preponderance in urban metros (5.2%), is also higher in widows (5.2%); the lower socioeconomic quintile shows a disproportionately higher incidence of alcohol use disorder, MDD and neurotic (stress) conditions.[2]
It is not surprising that the treatment gap that is, the number of persons who do not get adequate treatment for mental disorders is vast – alcohol abuse (86.3%), MDD (85.2%), bipolar disorder (70.4%) and neurotic conditions (83.2%).[2] Mental illness is widely stigmatised, which affects the subjects as well as their families at all levels – access to education, jobs and social interactions, including marriage. If this is the degree to which any sort of help cannot reach those in need, what can we say of homoeopathic help, which holds so much promise but is not widely known as a therapeutic option.
BARRIERS TO ACCESSING MENTAL HEALTH RESOURCES
Apart from the above mentioned social stigma that acts as a social barrier, one of the most potent blocks is that: Mental Health has always been a lower priority in public health policy, due to which it does not get the required funding. In low-middle-income countries, where the prevalence of mental illness is approximately 14.5%, the proportion of the health budget devoted to mental health is a paltry 2.62%.[7] The situation is not much better in the more developed countries where the burden is much greater without commensurate allocation of resources. However, we can assume that the insurance system works somewhat better there compared to India; while mental illness should be covered by health insurance policies, the reality is different[8,9]
There is an inherent complexity to structuring Mental Health services. Moreover, there has been a paradigm shift in the ideas for managing mental illness over the past 50 years.[10] Increasingly, the notion that treatment is best delivered in mental hospitals (formerly called asylums) has been challenged; communitisation of these services has been found to be more effective.[11] This involves significant investment in human resource training and producing skilled mental health workers who can cater to the problems as they arise in the community. This involves decentralisation; unfortunately, the bureaucracy is most comfortable with the opposite. Only recently did the State Government of Maharashtra announce the setting up of a Mental Hospital over 16 acres at a cost of Rs. 150 crores to cover patients across three districts of Marathwada. It is tempting to recall the heydays of homoeopathy in the 19th Century United States where it was reputed to have been able to empty mental asylums
Considering the above mentioned points, primary care psychiatry needs to be delivered at the primary health centres. Are these places equipped for the task? A study carried out by NIMHANS was revealing.[12] Primary care physicians trained by NIMHANS personnel in primary care psychiatry were evaluated through a well-designed process. The physicians could manage the diagnostic aspects well in most cases. However, the use of psychotropic drugs left a lot of lacunae, resulting in suboptimal treatment. This is not surprising since the undergraduate syllabus in allopathic (and homoeopathic) courses has dealt perfunctorily with the teaching of psychiatry. The graduate is therefore ill-equipped to understand and manage the complexity of psychiatric conditions
Lack of trained psychiatric personnel at all levels of mental healthcare delivery points is a worldwide phenomenon.[13] In the NMHS survey, except for Kerala, where the availability of psychiatrists (per lakh population) was 1.2, all others were far short of the minimal one psychiatrist per lakh of population.[2] Kerala also had the highest number of clinical psychologists (0.6 per lakh population). The availability of psychiatric social workers was relatively low across all the NMHS states. It is clear that waiting for the system to provide trained professionals is going to take ever so long while the mental issues continue to grow. Some bold efforts have been made to train a cadre of community mental health workers from the population.[14,15] The idea has yet to catch on.
PROMISE OF HOMOEOPATHY TO CATER TO THE PROBLEMS IDENTIFIED AND THE BLOCKS
As homoeopaths, we feel confident of the ability of our science to deliver in all areas, including the treatment of mental illness. Some of this promise centres around the following ideas we hold dear:
It is holistic and hence does not separate the mental and physical aspects of health
It is effective at both levels
It has no side effects
It is patient friendly and easy to administer
It is one of the most economic medicinal systems
It is green.
The problem emerges when we examine the attitudes to homoeopathy of those who matter in giving us free access to public mental health facilities. We find they do not care much for our ideas. To an objective observer, the blocks are formidable:
Homoeopathic treatment needs considerable investment in training the physician to individualise and prescribes accurately. The number of prescriptions is almost as many as there are homoeopaths. This defies common sense and shatters the confidence of those who would like to see some standardisation in clinical practice. As we know, individualisation reigns supreme not only with respect to the patients but also with respect to our clinical operations. This is not a workable proposition when we enter the public health arena
Clinical facilities are poor, especially for training in diagnosis and treatment of mental disorders. This holds true even in some postgraduate colleges where homoeopathic psychiatry is taught. This does not shore up the confidence needed for managing difficult illnesses
Acceptable research evidence regarding the treatment of mental illness is low. We have seen this phenomenon playing up in a number of epidemics, COVID-19 being the most recent example. It takes a lot to convince homoeopaths of the dictum Publish or Perish
Support from the Homoeo Pharma industry for research is poor. This is in stark contrast to the situation in the allopathic field, with almost every postgraduate department engaged in drug trials. Understandably, we enter into a vicious cycle of poor funding, leading to poor quality of research, which, in turn, yields very few publications.
As responsible professionals, wishing to make an impact on the pressing health issues of the day, we must plan and implement changes across the spectrum. How may we go about tackling these seemingly unscalable obstructions?
AVENUES FOR ENTRY TO HOMOEOPATHY AND HOMOEOPATHS IN MENTAL HEALTH
-
The National Mental Health Programme was launched in 1982 and has undergone updating through the years. The District Mental Health programme was launched in 1996 and is the primary means to reach out to the end user. It is unique in the sense that it outlines in an unprecedented way the approach to Community Mental Health.[16,17] Its main components are outlined in [Figure 1].
As one can see, the activities to be mounted under the programme are ones in which homoeopathic institutions/associations can get involved in an individual capacity or through associating with other mental health institutions or the district administration. Are there any supportive documents we can fall back upon?
The legal position of homoeopaths and homoeopathic psychiatrists in the Mental Health Act, 2017
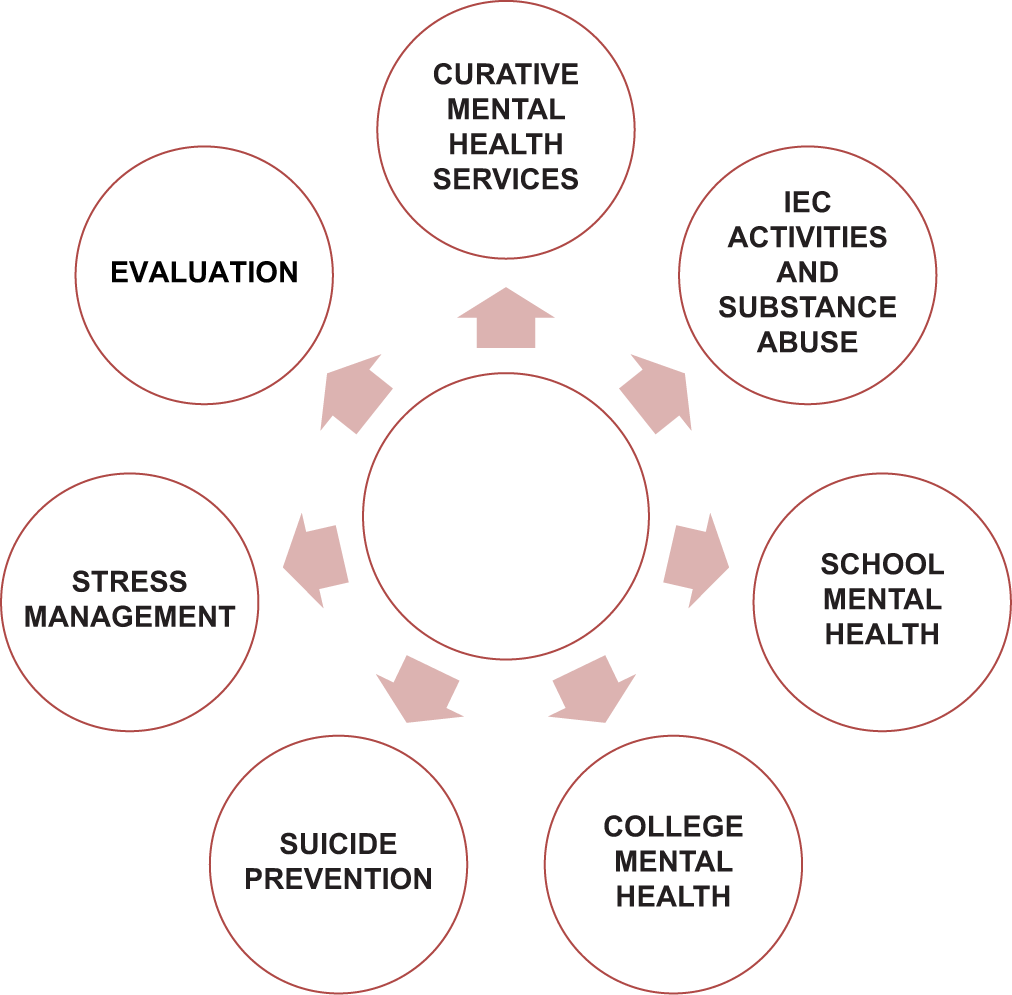
- Components of the District Mental Health Programme.
We are aware that the Mental Health Act, 2017, was passed after extensive consultations with all sections of the profession and civil society groups.[18] It is a progressive legislation in several important respects and breaks new ground, especially with respect to patient rights and providing advanced care provisions.[19] One significant change is the acceptance of all qualified AYUSH practitioners as Mental Health Professionals and the AYUSH Institutions catering to the mentally ill as eligible for being recognised as Mental Health Establishments under the Act. This enables the homoeopaths qualified as homoeopathic psychiatrists to discharge their duties under the act. However, as usual, there is a considerable lag between passing the laws and their implementation on the ground. We will do well to keep this in mind while approaching the authorities to gain access to facilities hitherto denied to homoeopaths.
With all this in our awareness, what sort of initiatives have been/can be undertaken by homoeopathic institutions to make their presence felt in the arena of Mental Health? The rest of this article showcases these for all of us to take cues and initiate similar programmes.
INITIATIVES BY HOMOEOPATHIC INSTITUTIONS IN THE ARENA OF MENTAL HEALTH
We will try to cover the relevant areas of intervention pertaining to the District Mental Health Programme.
IPD and OPD psychiatry
While the Mental Health Act, 2017, enjoins the setting up of certified Mental Health facilities, homoeopathic hospitals can do their bit to cater to the demand for outpatient and inpatient care of those affected. The Neuropsychiatry Department of the Rural Homoeopathic Hospital, Palghar, has been one of the four departments recognised as Centre of Excellence in Homoeopathy by the Ministry of AYUSH since 2012 and it has been having a closed Psychiatry ward (named the Anukampa Ward in an effort to destigmatise mental illness) since 2014.[20] More than 1000 patients have been treated in the ward from 2014 to 2018.[21] The outcomes of homoeopathic treatment in the ward have also been studied; a report is under publication. This facility has now been extended to geriatric patients as well.
School mental health
Since the inception of the homoeopathic psychiatry postgraduate programme in 2004, the department has been active in instituting various school mental health programmes in schools in the Palghar area.[22] This has resulted in a number of postgraduate students taking up this area for their dissertations; one such study is being published in the same issue of JISH as this manuscript.[23] Over the years, the interventions have been consolidated in the form of a report on homoeopathy in school mental health.[24] This work has extended to stress management in schools as well as identification of mental health issues in junior college students.
Research in mental health, especially in children
A number of neuropsychiatric conditions in children do not have any safe and effective allopathic treatment. Parents are generally reluctant to subject their wards to what is termed as chemical treatment and approach homoeopaths for help. Several conditions lend themselves to homoeopathic interventions and carefully planned research studies can yield a treasure trove of gains.[25-27] All three papers point to the benefit of homoeopathic intervention in learning disabilities and all grades of autistic spectrum disorders. Interested parent groups exist for these conditions (e.g., the Dyslexia Association); they can take advantage of these studies and popularise these interventions.
Community awareness regarding substance abuse and homoeopathic interventions
We have seen above the heavy burden of substance abuse in our population. It is incumbent on sensitive and aware mental healthcare institutes to carry the message of the dangers of addiction to all sections of the community. The activities of Information, Education and Communication can be carried out on several occasions.[28] Overtime, these awareness camps, street plays and well-publicised camps in the community and in the institutions can increase the inflow of patients; this, in turn, may enable publication of the results of homoeopathic intervention.[29] It is important that such studies are reported and published so that evidence for the efficacy of homoeopathic intervention builds up.
Training of volunteers for mental health
The shortage of trained professionals in the field of Mental Health has been alluded to above. The innovative and bold efforts of a few pioneers have also been mentioned. Our Psychiatry Department made considerable efforts in this direction, which were unfortunately interrupted by the onset of the COVID-19 pandemic in March 2020.[30] A total of 70 volunteers from the degree college were trained and 180 teachers were sensitised. The idea was that these volunteers would take care of the new entrants in the junior college so that the stress of newcomers would be eased and early referrals would take place. The results were encouraging and worth taking forward now that the pandemic is on the wane.
Enhancing awareness of women’s role in the community
Women often have inadequate access to mental healthcare. Programmes for, say, Women’s Day (8 March) are a great opportunity to connect to them in various forums and get the message of health, hygiene, social upliftment and the role of homoeopathy in improving their quality of life. The institute makes it a point not only to host in-house programmes to enhance their role but also spread the message in the community.[31] Colleges, Mahila mandals (Women’s organisations) and self-help groups predominantly comprising women are a fertile ground to plant these ideas. It is important to remember ‘When you empower a woman, you empower a Nation.’
Protecting mental health in senior citizen homes and in the community
The proportion of senior citizens is growing worldwide; they are another vulnerable section in the community. Often neglected, deprived and depressed, they stand to gain a lot from homoeopathic intervention for numerous ailments. First October, the International Day for Older Persons, can be an appropriate day for reaching out to them through activities/camps/workshops. Another vulnerable population are senior citizens living in old age facilities; the level of care available is not ideal in many of these places. This has only been exacerbated by the COVID-19 pandemic, due to the elderly population’s vulnerability to the illness and the social isolation it caused. As the article in this issue demonstrates, it is possible to mount interventions to improve the awareness of their strengths and build on their inherent capacities.[32] Homoeopathic intervention can be an additional bonus.
Training of homoeopathic undergraduates and physicians
We have already commented on the need to sensitise and train graduates, postgraduates and practitioners in all aspects of Mental Health and illness and the benefits of homoeopathic intervention. The current syllabus laid down by the erstwhile Central Council of Homoeopathy is inadequate and does not integrate the homoeopathic approach so powerfully stated in the Organon and elaborated on by other masters. The institute had an opportunity to draw up a novel curriculum for teaching psychology and psychiatry for homoeopathic undergraduate students. What was unique was that the postgraduate students of the institute were trained to deliver the teaching for the 2nd and 3rd and 4th years; the programme was a runaway success.[33,34] The programme, if replicated all over the country and combined with clinical exposure in the OPDs, promises to transform the mental healthcare scenario in the country. It is hoped that the National Commission of Homoeopathy will consider this innovative programme while it deliberates on its competency-based model of education.
Practitioners of homoeopathy also need to become aware of the further reach of homoeopathy in relieving mental distress and the manner in which this can be achieved. This is not an easy task since it demands careful curating of the clinical experience, clear establishment of the cause-effect relationships, ensuring that the thinking process demonstrated conforms to standard rules of evaluating symptoms, evolving the totality, assessing susceptibility and managing the posology along well-established lines. The series Fridays with Dhawale has been a remarkable achievement as it also transforms successful practitioners into successful guides.[35] Some of these talks have been transformed into articles that have attracted attention from prospective patients or their parents (in case of children) from different corners of the world.[36,37]
Utilising social media for mental health awareness
In this era, where a lot of business, education and entertainment happen through social media, we must employ it as an edutainment source for connecting to people everywhere with the sole purpose of communicating vital messages related to mental health. World Mental Health Day was one such occasion; the institute’s postgraduate students used it for spreading the message of mental health inequity and how this can be tackled.[38] The event garnered an enthusiastic response. Similarly, individual practitioners are taking to the medium to impart vital messages on popular topics, including drug intake and celebrity deaths by suicide.[39] This may seem like mere drops, but accumulation has to start somewhere. We must make a start; well begun is half done, as the saying goes.
RESEARCH PRIORITIES IN MENTAL HEALTH THROUGH HOMOEOPATHY
We need to raise reliable evidence to bring forth the benefit of homoeopathic intervention. It would be appropriate to focus on those clinical conditions that are common, relatively easily manageable on an outpatient basis, and that we as homoeopaths know have a favourable outcome. Chief among these are common mental disorders, childhood behavioural and learning difficulties, geriatric disorders and substance abuse conditions. The existing body of work worldwide can be buttressed with fresh evidence from India.
CONCLUSION
The world is undergoing a quick transformation in all areas, which is affecting all of us in myriad ways. One of the noticeable impacts is to our mental health. All data point out that the burden of mental illness is on the increase and the resources to combat it are woefully short.
Homoeopathy has a significant role to play in mitigating the distress. However, the current barriers need to be carefully understood and a multipronged effort needs to be launched at the grassroots level. There is evidence that when the task is undertaken with commitment and passion backed by sound knowledge and adequate skillset, we can make the desired impact. Quality clinical studies and research with homoeopathic intervention can communicate the ability of suitable trained homoeopaths to make a difference to the current mental health scenario and thus enhance our entry into integrated healthcare for alleviating mental distress.
Just as the climate change votaries claim, the time to act is now. So should homoeopathic psychiatrists also act now.
Acknowledgements
The article is based on a webinar talk delivered to the Homoeopathic Association of Psychiatrists in India on the occasion of World Mental Health Day, 2021. I am grateful to the organisers of the event for enabling me to present my thoughts on the day.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Promoting Mental Health: Concepts, Emerging evidence, Practice: A report of the World Health Organization, Department of Mental Health and Substance Abuse in collaboration with the Victorian Health Promotion Foundation and the University of Melbourne Geneva: World Health Organization; 2005.
- [Google Scholar]
- National Mental Health Survey of India, 201516: Summary Bengaluru: National Institute of Mental Health and Neuro Sciences, NIMHANS Publication No. 128; 2016.
- [Google Scholar]
- The burden of mental disorders across the states of India: The global burden of disease study 1990-2017. Lancet Psychiatry. 2020;7:148-61.
- [Google Scholar]
- Exploring the role of homoeopathy in the management of learning disabilities. The Homoeopathic Heritage. 2012;38:23-8.
- [Google Scholar]
- COVID-19 Mental Disorders Collaborators. Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in, 2020 due to the COVID-19 pandemic. Lancet. 2021;398:1700-12.
- [CrossRef] [Google Scholar]
- Resources for mental health: Scarcity, inequity, and inefficiency. Lancet. 2007;370:878-89.
- [CrossRef] [Google Scholar]
- Economic Times Can you buy Health Insurance Cover for Mental Illnesses? AM IST, E-Paper; 2021.
- [Google Scholar]
- Barriers to improvement of mental health services in low-income and middle-income countries. Lancet. 2007;370:1164-74.
- [CrossRef] [Google Scholar]
- Disappearing the asylum: Modernizing psychiatry and generating manpower in India. Transcult Psychiatry. 2016;53:783-803.
- [CrossRef] [PubMed] [Google Scholar]
- Mental health services provided by medical officers in primary health centres in Kolar district in Karnataka, India: A situational assessment. J Family Med Prim Care. 2020;9:173-9.
- [CrossRef] [PubMed] [Google Scholar]
- Digital training for non-specialist health workers to deliver a brief psychological treatment for depression in primary care in India: Findings from a randomized pilot study. Int J Environ Res Public Health. 2020;17:6368.
- [CrossRef] [PubMed] [Google Scholar]
- To Meet a 'Tsunami' of Need, a Daring Proposal to Train Thousands of Lay Mental Health Workers. 2020. Taking a Lesson from the Developing World. Available from: https://www.medium.com/california-state-of-mind/to-meet-a-tsunami-of-need-a-daring-proposal-to-train-thousands-oflay-mental-health-workers-b9450680607d [Last accessed on 2021 Nov 28]
- [Google Scholar]
- District Mental Health Programme. 2015. Available from: https://www.main.mohfw.gov.in/sites/default/files/56464578341436263710_0_0.pdf [Last accessed on 2021 Nov 28]
- [Google Scholar]
- District Mental Health Programme. 2011. Available from: http://www.aamh.edu.au/wp-content/uploads/2014/01/06_india_dc_jain.pdf [Last accessed on 2021 Nov 28]
- [Google Scholar]
- Mental Health Care Act 2017. 2017. Available from: https://www.egazette.nic.in/WriteReadData/2017/175248.pdf [Last accessed on 2021 Nov 28]
- [Google Scholar]
- Mental healthcare Act 2017: Need to wait and watch. Int J Appl Basic Med Res. 2018;8:67-70.
- [CrossRef] [PubMed] [Google Scholar]
- Available from: https://www.mldtrust.org/activities-ofanukampa-ward [Last accessed on 2021 Nov 28]
- Demographic and clinical profile of psychiatry patients of rural Homoeopathic hospital, Palghar, Maharashtra, India, from 2014 to 2018. Homoeopathic Links. 2021;34:106-11.
- [CrossRef] [Google Scholar]
- Available from: https://www.mldtrust.org/school-mental-health-programme-in-tarapore [Last accessed on 2021 Nov 28]
- Assessment and homoeopathic management of psychological stresses and somatic illnesses in high school students from rural Palghar: Observational case series. J Integr Stand Homoeopathy. 2021;4:112-9.
- [Google Scholar]
- Use of homoeopathic remedies in the management of learning disabilities. Indian J Res Homoeopathy. 2014;8:87-94.
- [CrossRef] [Google Scholar]
- Effectiveness of homoeopathic therapeutics in the management of childhood autism disorder. Indian J Res Homoeopathy. 2014;8:147.
- [CrossRef] [Google Scholar]
- Autistic spectrum disorder-holistic homoeopathy. Homoeopath Links. 2011;24:31-8.
- [CrossRef] [Google Scholar]
- Available from: https://www.mldtrust.org/community-awareness-activities-by-rhh [Last accessed on 2021 Nov 28]
- Homoeopathy in acute alcohol withdrawal syndrome: An exploratory study. Homoeopath Herit. 2013;7:21-7.
- [Google Scholar]
- Available from: https://www.mldtrust.org/mentalhealthvolunteers [Last accessed on 2021 Nov 28]
- Available from: https://www.mldtrust.org/college-outreachon-womens-day [Last accessed on 2021 Nov 28]
- Planning for mental wellbeing in an old age home during the COVID-19 pandemic by homoeopathic institution: Structuring the intervention. J Integr Stand Homoeopathy. 2021;4:106-11.
- [Google Scholar]
- Concept of mental health and disease for practical implementation: A case-based teaching for undergraduate students-Part I of basic and applied psychology. Homoeopathic Links. 2020;33:82-9.
- [CrossRef] [Google Scholar]
- Concept of Mental Health and Disease for Practical Implementation: A Case-Based Teaching for Undergraduate Students Part II: Abnormal Psychology and Psychiatry and the Homoeopathic Approach, Homoeopathic Links. 2020
- [CrossRef] [Google Scholar]
- Dr. ML Dhawale Memorial Homoeopathic PG Institute. FWD Talks. 2021. Available from: https://www.youtube.com/playlist?list=pl7o4t_cek_bj_ocf6pdngyupe-x7svjll [Last accessed on 2021 Nov 28]
- [Google Scholar]
- Homoeopathic management of dissociative fugue: A case report. J Integr Stand Homoeopathy. 2021;4:80-5.
- [CrossRef] [Google Scholar]
- Challenges faced in homoeopathic treatment in autism-a case series. J Integr Stand Homoeopathy. 2021;4:29-36.
- [CrossRef] [Google Scholar]
- Dr. ML Dhawale Memorial Homoeopathic PG Institute: World Mental Health Day. 2021. Mental Health in an Unequal World. Available from: https://www.youtu.be/syrv4_-lv5q [Last accessed on 2021 Nov 28]
- [Google Scholar]
- संवाद-A Dialogue within and without. 2021. Available from: https://www.youtube.com/channel/ucpcf38-x7ogmkidyw2uaopw [Last accessed on 2021 Nov 28]
- [Google Scholar]







